-
Plastic Surgery
View All
Plastic Surgery
- Face
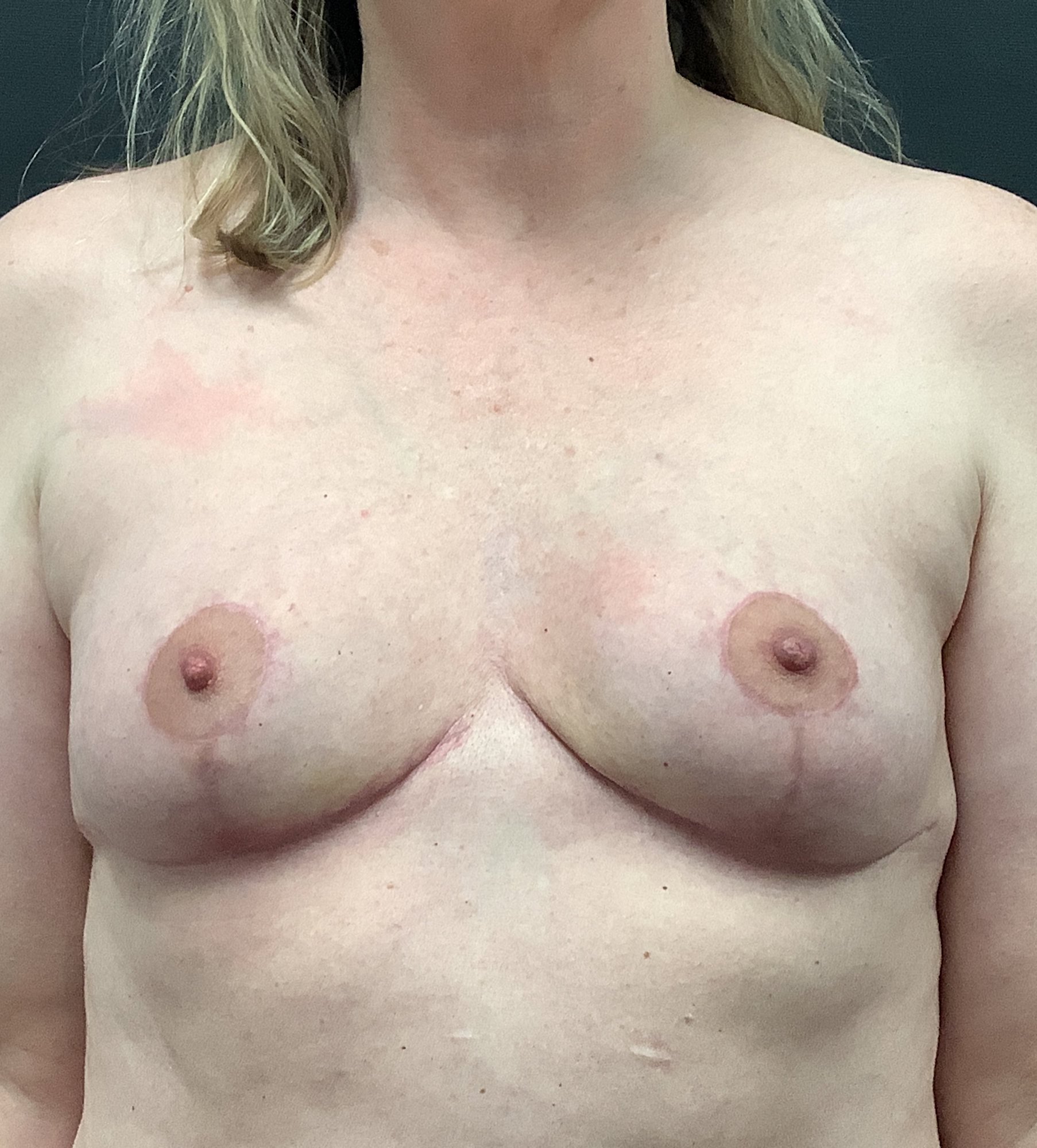
- Breast
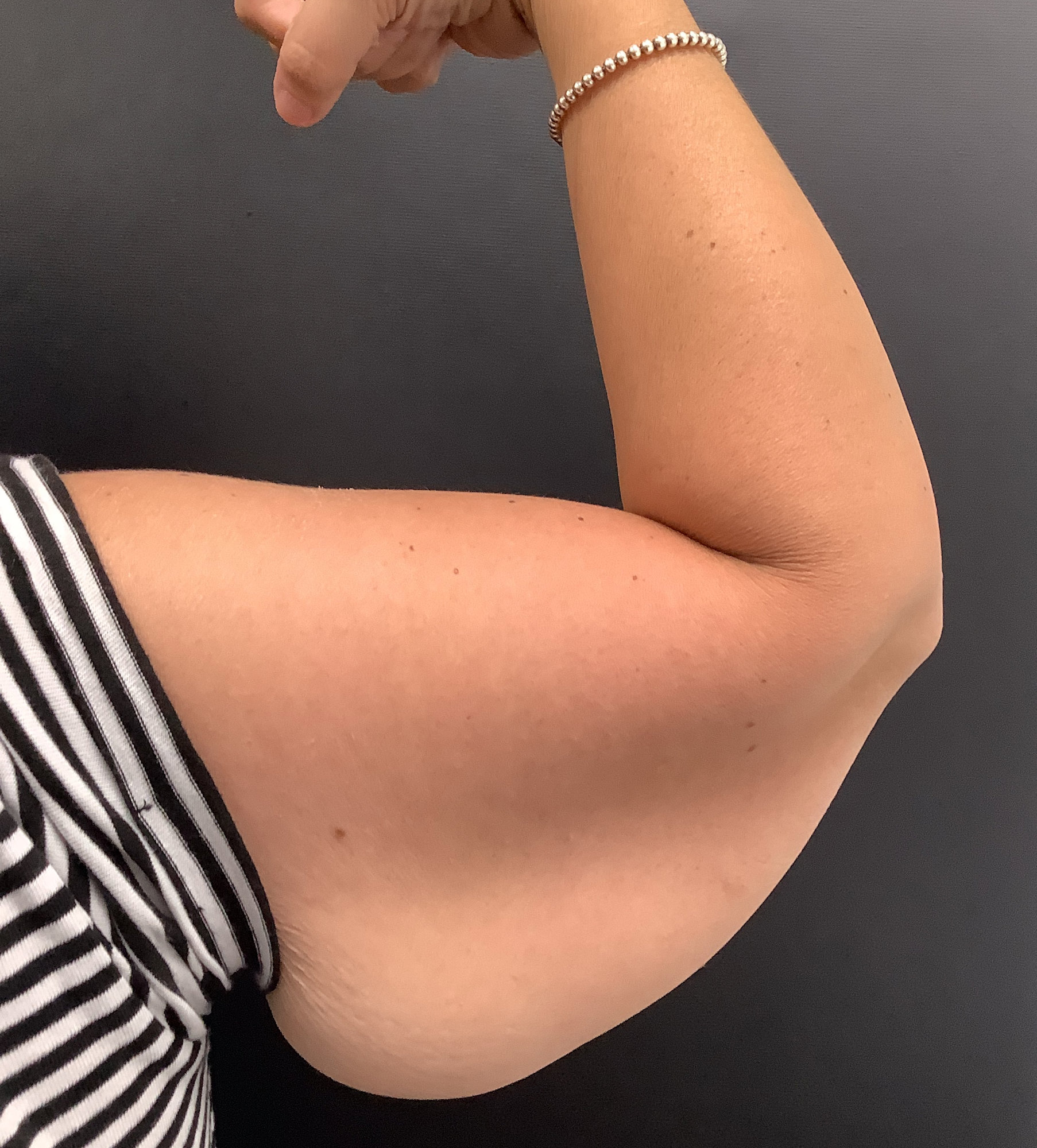
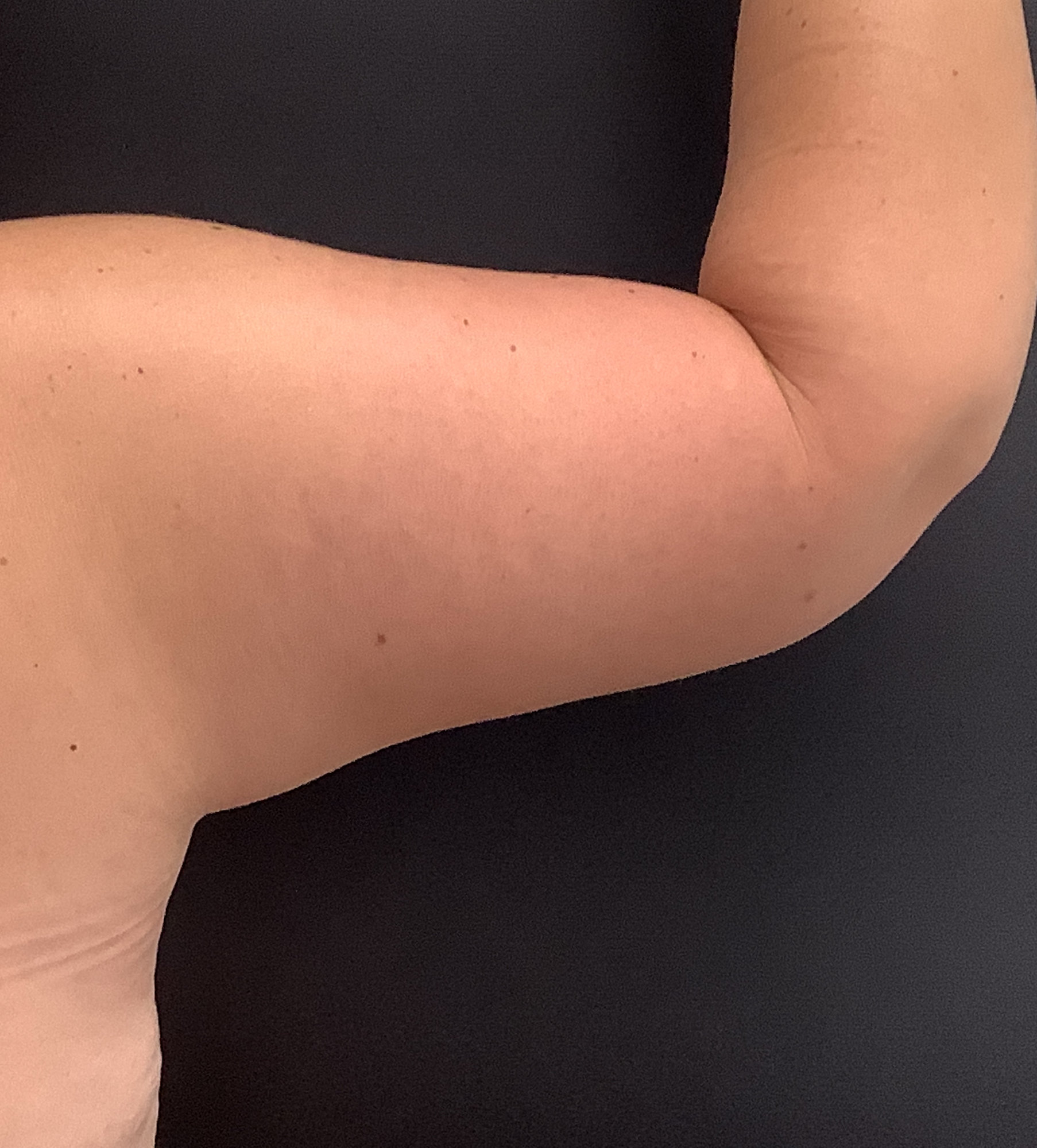
- Body
- Vaginal Rejuvenation
- Transgender Services
-
Aesthetic Treatments
Aesthetic Treatments
- Injectables
- Lasers
- Body & Vein
- Skin Rejuvenation
- Hair Restoration
- About PSC
- Patient Resources
Plastic Surgery and Med Spa in Wichita
Welcome to the Plastic Surgery Center and PSC Aesthetics. We’re committed to helping you look and feel your best.
The Plastic Surgery Center in Wichita, Kansas, is the longest standing private plastic surgery practice and med spa in Wichita & the state of Kansas.
For more than 50 years, our mission has been—and continues to be—to provide the highest quality of care along with the highest standard of safety and technical expertise to our patients. Our doctors, nurses, and skincare providers are dedicated to the care of you: our cosmetic, reconstructive, and skincare patients.
We know choosing to have plastic surgery or a skincare procedure is a personal decision.
As your trusted provider, you can count on us to help you achieve your goals. With impeccable credentials and ongoing continuing education, you will find the most qualified staff in Wichita and the greater Midwest area to help you look and feel your best.

What We Do
Your Journey Starts Here
Plastic Surgery
You deserve fabulous results in a safe, secure, and comfortable environment.
You'll find two board-certified plastic surgeons, Amy Sprole, MD, FACS, and Joe Spaniol, MD. They provide real results you can trust in both cosmetic and reconstructive surgery of the face, breast, and body. From your first consultation all the way through surgery and recovery, you experience the highest quality care, safety, and service.
You'll find two board-certified plastic surgeons, Amy Sprole, MD, FACS, and Joe Spaniol, MD. They provide real results you can trust in both cosmetic and reconstructive surgery of the face, breast, and body. From your first consultation all the way through surgery and recovery, you experience the highest quality care, safety, and service.
Aesthetics
If you're not quite ready for surgery, you will find a skincare department comprised of two registered nurse injectors, an aesthetics injector, and two medical aestheticians.
These experts provide minimally and non-invasive skin care of the face and body including injectables, fillers, laser treatments, and more.
These experts provide minimally and non-invasive skin care of the face and body including injectables, fillers, laser treatments, and more.
Wellness and Weight Loss
You have access to an extensive menu of solutions targeted and individualized for all your wellness and weight loss goals.
Looking to lose weight? Your highly qualified plastic surgeons can provide the Orbera weight loss balloon, Endoscopic Suture Gastroplasty (ESG), and Transoral Outlet Reduction (TORe) for nonsurgical gastric bypass revision.
Our wellness department can help with Semaglutide, Tirzepatide, and Lipo B injections for weight loss, IV therapy for mineral deficiencies,
Looking to lose weight? Your highly qualified plastic surgeons can provide the Orbera weight loss balloon, Endoscopic Suture Gastroplasty (ESG), and Transoral Outlet Reduction (TORe) for nonsurgical gastric bypass revision.
Our wellness department can help with Semaglutide, Tirzepatide, and Lipo B injections for weight loss, IV therapy for mineral deficiencies,
Medical-grade skincare products are more powerful than drugstore brands. You can now buy online!
Wondering about skincare packages at our own PSC Aesthetics? Check them out now!
You’ll find products designed to meet your needs at any age. Find acne, anti-aging, and moisturizing products in our online shop!
Ready to start your weight loss journey? We offer the Skinny Shot!
With options including Semaglutide and Tirzepatide, we can help you meet your weight loss goals!

Meet Our Doctors •
Our plastic surgeons, Amy Sprole, MD, FACS, and Joe Spaniol, MD, all provide the full spectrum of plastic surgery procedures. They specialize in cosmetic and reconstructive surgery of the face, breast, and body.
With exceptional education, training, and experience, they are trusted to provide you with safe, fabulous results.
Plastic Surgery Center
Featured Specials
Monthly Special
Lash Extensions Special
Monthly Special
Wellness and Weight Loss Special
Monthly Special
Cool Month is Here

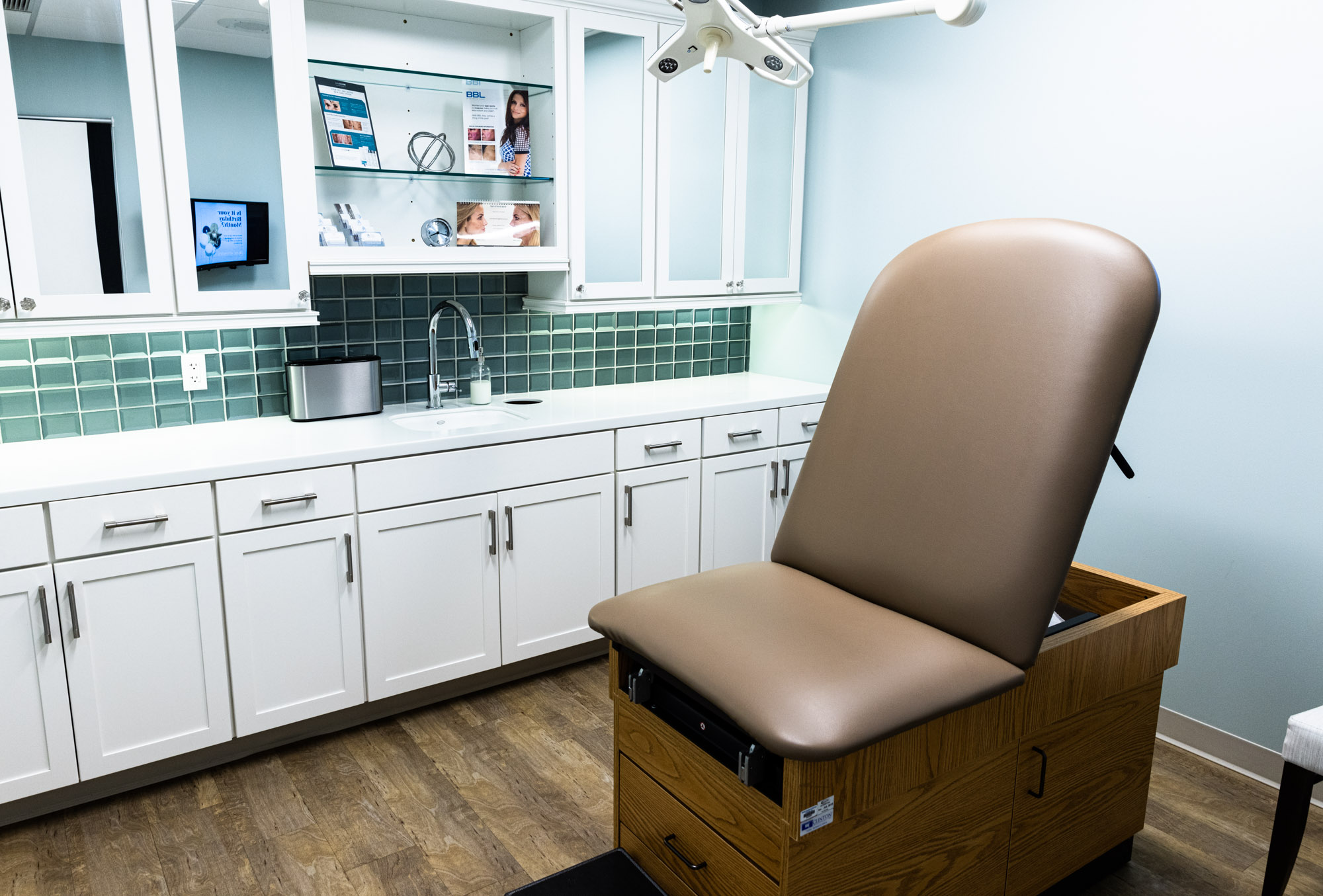
The PSC Experience
Expect Only the Best
When you walk in the doors of the Plastic Surgery Center and PSC Aesthetics plastic surgery and med spa in Wichita, you’ll find a warm, comfortable, and relaxing atmosphere with staff ready to help you meet your surgical and skincare goals.
You’ll find the highest quality service, the utmost in expertise, privacy, and overall safety. You can count on outstanding results every time.
Virtual Consultation Tool
What’s Best for You?
Want to learn more? Use the virtual consultation tool below. If you are ready to schedule your consult with one of our plastic surgeons, contact us today.
Resources
Looking for answers? Check out the following resources:
Highly Trained Plastic Surgeons
East Wichita Office
Address
1861 North Webb Road
Wichita, KS 67206
Phone
316-688-7500
Hours
Monday 8 am – 4:30 pm
Tuesday 8 am – 4:30 pm
Wednesday 8 am – 4:30 pm
Thursday 8 am – 4:30 pm
Friday 8 am – 4 pm
Saturday By Appointment Only
PSC Aesthetics offers evenings and weekend appointments

West Wichita Office
Address
3931 North Ridge Road
Wichita, KS 67205
Phone
316-588-9220
Hours
Monday 8 am – 4:30 pm
Tuesday 8 am – 4:30 pm
Wednesday 8 am – 4:30 pm
Thursday 8 am – 4:30 pm
Friday 8 am – 4 pm
Saturday By Appointment Only
PSC Aesthetics offers evenings and weekend appointments

Gift certificates for the Plastic Surgery Center and PSC Aesthetics are available for purchase!
You may stop by and purchase one in person, or use the button below to purchase an online gift certificate. You can also elect to have the certificate emailed to a gift recipient. If you have any questions, please give us a call at 316-688-7500.